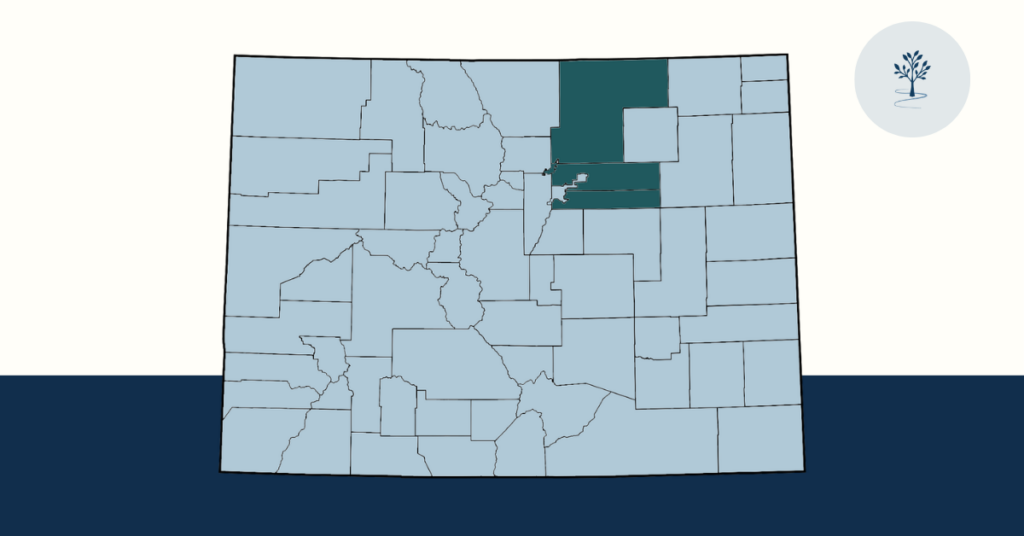
If you live in Northern Colorado, you may have already seen the headlines: a measles case has been confirmed in Weld County, with a potential exposure at UCHealth Medical Center of the Rockies in Loveland. This is not cause for panic — but it is a good time to make sure you and your family are protected, know what to watch for, and understand when to reach out to your doctor.
At Rellas Family Medicine, we believe informed patients are healthier patients. Here’s what you need to know.
What's Happening With Measles in Colorado Right Now
A confirmed case close to home
On March 18, 2026, Colorado public health officials confirmed a measles case in a Weld County adult who had not been vaccinated and had recently traveled out of state to an area with an active outbreak. The individual was hospitalized and has since been discharged. Anyone who was at the UCHealth Medical Center of the Rockies emergency department in Loveland on March 17, 2026 between 5:30 a.m. and 1:30 p.m. may have been exposed.
This case is separate from the ongoing outbreak centered in Broomfield, where more than 10 cases have been confirmed — primarily among unvaccinated school-age children.
Colorado and national context
- Colorado recorded 36 measles cases in 2025 — the most in a single year in over a decade, and a dramatic increase from recent years when the state typically saw zero to two cases annually
- Nationally, more than 1,300 confirmed measles cases have already been reported in 2026, surpassing the 2019 high-water mark of 1,274 cases — and we’re only in March
- 93–97% of confirmed cases nationally involve people who were unvaccinated or whose vaccination status was unknown
What's Happening With Measles in Colorado Right Now
Measles is not a mild illness
Measles is one of the most contagious diseases that exists. If one person is infected, up to 9 out of 10 unvaccinated people nearby will contract it. The virus can survive in the air or on surfaces for up to two hours after an infected person has left a room — meaning you can be exposed without any direct contact.
Potential complications
For many healthy adults, measles causes a miserable but survivable illness. But for others — particularly young children, infants under 12 months, pregnant women, and anyone with a compromised immune system — it can be serious. Potential complications include:
- Pneumonia (a leading cause of measles-related death in children)
- Encephalitis (brain swelling), which can cause permanent disability or death
- Hearing loss
- Premature birth or miscarriage in pregnant women
- In 2025, measles killed three people in the United States
Measles is never routine. It was never a “right of passage.” It’s a serious, preventable disease — and that’s exactly why the vaccine was developed.
Measles Symptoms: What To Watch For
Timeline matters
One of the most challenging things about measles is that the incubation period — the time between exposure and symptoms — ranges from 7 to 21 days. That’s a wide window, and during part of that time, an infected person is already contagious without knowing it. People with measles are contagious from four days before the rash appears through four days after it clears.
Early symptons (days 1-4)
The early stage of measles looks a lot like a bad cold or flu. Watch for:
- High fever (often 104°F or higher)
- Persistent cough
- Runny nose
- Red, watery eyes (conjunctivitis)
- A general feeling of being very unwell
Koplik's spots — the distinctive early sign
A few days into the illness, small white or bluish-white spots may appear inside the mouth, on the inner cheeks. These are called Koplik’s spots and are a hallmark sign of measles. If you see them alongside the other symptoms above, contact your doctor before going anywhere.
The rash
Around day 3–5 after symptoms begin, the measles rash appears. It typically:
- Starts at the hairline and spreads down the face
- Then moves down the neck, trunk, arms, and legs
- Appears as flat red spots that may merge together
- Can last 5–6 days
By the time the rash appears, the person has usually been contagious for several days.
When to see call your doctor
If you or your child develops a high fever with a cough, runny nose, and red eyes — especially if you were at the Loveland UCHealth ER on March 17 or have been in a known exposure location — do not go directly to a clinic or emergency room. Call ahead first. This is critical to prevent spreading the virus to other patients, including vulnerable infants and immunocompromised individuals
RFM members:
Message Dr. Rellas directly on Spruce. That's exactly what direct access is for.
How to Protect Your Family
Vaccination is the single most effective protection
Two doses of the MMR (measles, mumps, and rubella) vaccine are approximately 97% effective against measles. The standard schedule is:
- First dose at 12–15 months
- Second dose at 4–6 years
Not sure if you're up to date?
You can request your vaccination record — or your child’s — through the Colorado Immunization Information System (CIIS) self-serve portal at cdphe.colorado.gov. If you’re unsure, err on the side of checking. It’s a quick process and gives you peace of mind.
What to do if you were potentially exposed
If you were at a known exposure location and are unvaccinated, getting the MMR vaccine within 72 hours of exposure may prevent illness or reduce its severity. Contact your doctor as soon as possible. Do not wait to see if symptoms develop before reaching out.
Special considerations
- Infants 6–11 months who live in or are traveling through outbreak areas may be eligible for an early MMR dose — talk to your doctor
- If you are pregnant and unsure of your immunity status, contact your OB or primary care physician now, before any potential exposure
- Immunocompromised individuals should speak with their care team about specific guidance
Measels FAQs
Q: Is there a measles outbreak in Fort Collins right now?
A: As of March 2026, there is an active measles outbreak in the Broomfield area of Colorado, and a separate confirmed case in Weld County with a potential exposure site in Loveland. Fort Collins has not confirmed a case at this time, but given the proximity and the nature of how measles spreads, it’s a good time for all NoCo families to check vaccination status and know what symptoms to watch for.
Q: What are the first signs of measles?
A: Early measles symptoms look like a bad cold or flu: high fever, cough, runny nose, and red, watery eyes. A few days in, small white spots may appear inside the mouth (Koplik’s spots). The characteristic red rash typically appears 3–5 days after symptoms begin, starting at the hairline and moving downward.
Q: How long does it take for measles symptoms to appear after exposure?
A: The incubation period for measles is 7 to 21 days. During that window — especially in the days just before the rash appears — a person can already be contagious without knowing it.
Q: Can you get measles if you’ve been vaccinated?
A: It’s possible but uncommon. Two doses of the MMR vaccine are about 97% effective. A small number of vaccinated people can still contract a milder form of the illness, but the vaccine dramatically reduces both the risk of infection and the severity of illness.
Q: What should I do if I think I’ve been exposed to measles?
A: Call your doctor before going to a clinic, urgent care, or ER. This is important to prevent spreading the virus to other vulnerable patients. If you are unvaccinated, getting the MMR within 72 hours of exposure may help prevent or reduce illness. RFM members can message Dr. Rellas directly on Spruce for guidance.
Q: Is the MMR vaccine safe?
A: Yes. The MMR vaccine has decades of safety data and is one of the most well-studied vaccines available. Two doses provide approximately 97% protection against measles. The risks of the vaccine are far smaller than the risks of measles itself.
Q: My child is under 12 months — are they protected?
A: Infants under 12 months are too young for the standard MMR schedule and are among the most vulnerable to serious measles complications. If you live in or near an outbreak area, talk to your pediatrician or family doctor about whether an early dose is appropriate.